
We Often Take Our Health for Granted Until It’s Gone
This week, I underwent a microdiscectomy, and today, I’m back at home.
Eighteen days ago, I bent over to pick up a billiard ball while playing pool, and my back went into spasms. After four days of attempting to manage the pain with medication prescribed by my
GP and following advice from my physiotherapist, I was admitted to the hospital, where I’ve spent just over two weeks. I had been experiencing excruciating and nearly constant pain for the past 18 days due to nerve pain in my left leg caused by a bulging disc at the L5/S1 level. Remarkably, I no longer feel any pain in my leg, and there’s only minor discomfort in my back from the surgery
. For nearly the entire duration of this ordeal, I couldn’t walk more than a few steps without experiencing intense pain. However, today marks a significant change as I can now walk completely pain-free. It’s an incredible feeling, and though I’m still somewhat weak from the experience and the lack of movement during my hospital stay, I’m filled with gratitude for those who have supported me. This experience has compelled me to reflect upon it and share my thoughts with you.
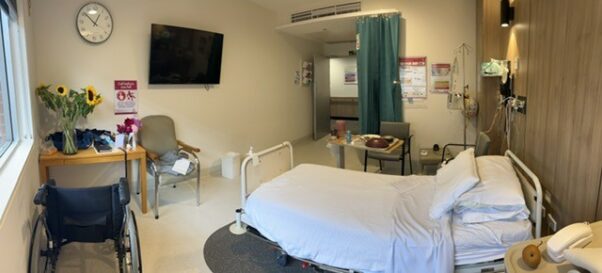
This was the room I have lived in for 14 days without going outside.
Accepting help is sometimes hard, particularly for men.
All my life I have been the one to take care of others. I get a great deal of satisfaction from helping others, whether that be my family and friends or through my role as an Organisational Psychologist. However, this is probably the first time in my life when I’ve needed help for a prolonged period of time. It is sometimes hard to accept help from others for me, but I think I’ve learned to accept and appreciate help. Sharing my pain with others and being totally vulnerable has been a good thing. It has led to the empathy and incredible support I have received from friends and family. I’d like to sincerely thank the inspiring author Brene Brown for teaching me about ‘The Power of Vulnerability‘.
I’ve been amazed and humbled by the support I’ve had and how this has impacted my social wellbeing.
Many people have sent messages of love and support; people have come to visit me in the hospital. I’ve got flowers, chocolates, and many more gifts of love and affection; so while my physical wellbeing has been hampered, in many ways, my social wellbeing is better because I feel the love from friends and family. Notwithstanding this, even as an extrovert, I was fascinated to find that when the pain was at extreme levels, I wanted to be alone. I did not want to see people. I was in no state to even try to hold a conversation with others, even close friends or family. So, context for social wellbeing is crucial, and some alone time for various reasons is important, although too much of this will not be helpful, and hiding away in isolation for too long is unhealthy. I wonder how the context and circumstances impact our need for social connections with others? What factors drive us to need more social connections and what parts of life require us to be alone for a little while? Furthermore, emotional wellbeing was significantly reduced during this period in the hospital because it was incredibly draining, and the pain was almost totally continuous, so I struggled to cope emotionally and spent numerous mornings crying to myself after another terrible night without sleep. However, today I feel my emotional wellbeing has increased significantly, and I feel it is definitely related to the support I have received over these last few weeks and to the fact that I had my first decent night’s sleep in 18 days last night.
To manage the pain, beyond the heavy medication I was receiving, I did my own breathing and relaxation techniques.
I’ve used and practiced many different relaxation methods for over 30 years. I teach it to others. I noticed that when the pain was extreme, I struggled to focus on my breathing to bring the pain levels down. However, when it was only medium-level pain, the breathing and relaxation techniques I used were helpful in minimizing the level of pain I experienced. When I thought about breathing techniques specifically for pain management, I learned that I need to stop resisting the pain and trying to fight it because this only increases the tension around the pain areas and instead try to embrace the pain, focus on it, and aim to use visualization to soothe the pain and use breathing while focusing on the pain areas and seek to ask those pain areas to let go and relax as much as possible. I did find that this was helpful. I’m curious to know if others have had similar experiences where breathing or relaxation techniques are harder to use when in significant pain? These techniques require you to be able to focus your attention on something (e.g. your breath), but I found I struggled to do this very well when the pain was extreme, but I could do it when the pain was less severe. What have you found?
Most of the work I do with the company I run – Steople – is about helping other individuals or teams to change their habits and behaviors in ways that stick.
I’ve worked hard on ‘walking the talk’ and living a healthy, well, and fulfilling life. This experience has given me further insights about myself that I was aware of but not changing – we call that the ‘knowing-doing gap’. Many people have told me NOT to overdo it and to take it easy (most of these people know me well and know I sometimes push myself too hard). I have known for a few years now that I need to work harder at managing the sport and exercise I do so that I do not injure myself. I’ve always been proud of the fact that I’m extremely fit and healthy for a 56-year-old man, and I don’t want my age to set too many limits on what I can do physically. However I also need to be a little bit more realistic and ensure the activities I do are not going to cause me further injuries. So, I think I have learned that motivation is a key ingredient for anyone to change their behaviors. I’ve been aware of this habit for years, but now I feel I have more motivation to make the necessary changes. I will need to channel lessons from BJ Fogg’s book on Tiny Habits: The Small Changes That Change Everything and create what he called ‘laughably small’ changes to my habits to help me move towards my new goal.
A final reflection from this experience is about a different factor involved in changing habits.
In order to grow and develop in deeper ways, we need to experience some level of discomfort. Scott Carney in his thought-provoking book called What Doesn’t Kill Us: How Freezing Water, Extreme Altitude, and Environmental Conditioning Will Renew Our Lost Evolutionary Strength (2017) was able to provide strong evidence about how we need to experience physical discomfort through incrementally increasing our exposure to challenging and cold environments in order to build our immune system and become stronger. While this experience in the hospital was not cold-water exposure therapy, I certainly have been physically, mentally, and emotionally uncomfortable over the last few weeks. So what have I learned? I’m not really sure but I think I always had an awareness that I sometimes push myself too hard, but I perhaps have learned WHY I need to change this habit. Perhaps this new level of motivation to change this aspect of me will help me move from knowing about this to doing something differently? We’ll see.
These are my reflections on the day I have left the hospital after over 2 weeks of excruciating pain. They are reflections about myself and an attempt to link my experiences with what the research tells us about health, wellbeing, and changing habits. I would love to hear other people’s views on my reflections to help us all build a deeper understanding of some of these nuances involved in taking care of ourselves.

This was one of many nurses who looked after me every day and night.

